Nail Psoriasis: How to Spot It and What to Do
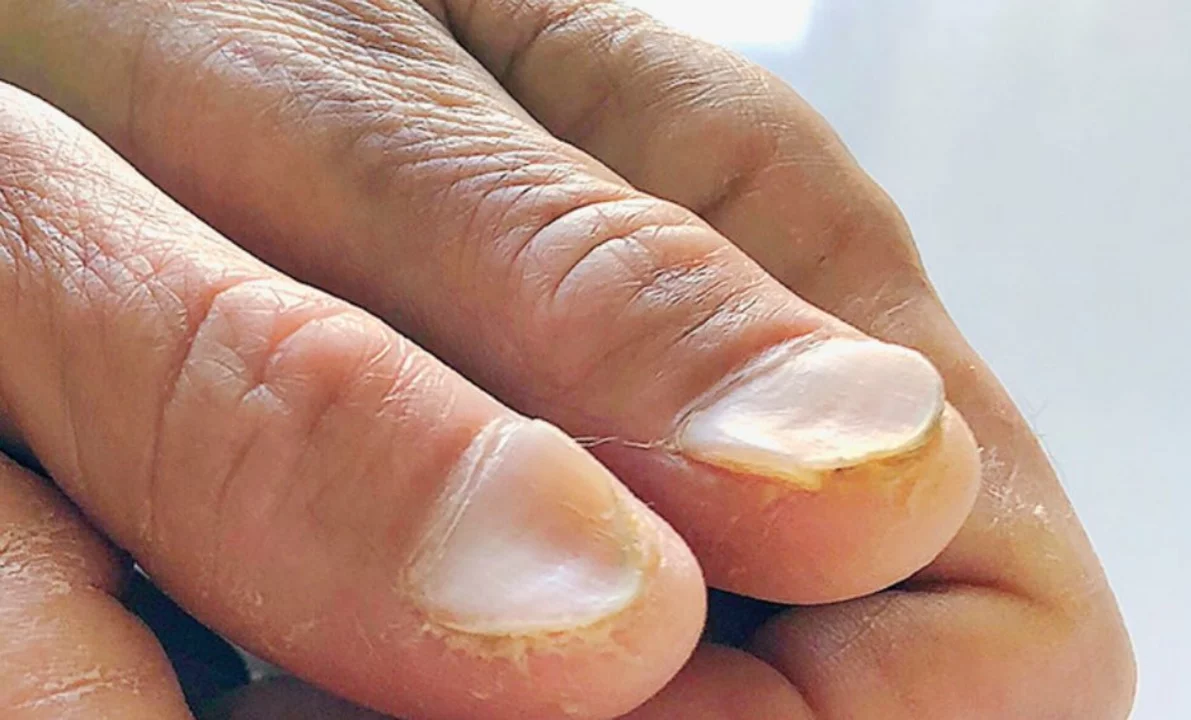
Nail psoriasis can wreck the look and function of your nails long before skin patches show up. If your nails have pits, lift off the nail bed, or show a yellow-brown "oil drop" stain, you might be dealing with nail psoriasis. It’s common, stubborn, and slow to heal — but knowing what to expect makes a big difference.
Causes & common signs
Psoriasis is an immune-driven condition that speeds up skin cell turnover. When this happens in the nail matrix (where the nail forms) or the nail bed, you get visible changes. Look for these classic signs: small pits in the nail surface, white or yellowish spots (oil drop), onycholysis (the nail lifting away from the nail bed), thickening or crumbling, and buildup under the free edge called subungual hyperkeratosis. Fingernails usually grow out faster than toenails, so results show earlier on hands.
Sometimes nail changes are the only sign of psoriasis. They can also be an early clue to psoriatic arthritis, so if you have joint pain along with nail issues, see a specialist.
Treatment options and everyday nail care
Treating nail psoriasis takes patience — nails grow slowly. Fingernails need 3–6 months to show improvement; toenails can take a year or more. Treatments depend on where the problem sits (matrix vs. bed) and how bad it is.
Topical treatments: High‑potency steroid creams or ointments and vitamin D analogs (like calcipotriol) are used directly on or around the nail. Results are modest but worth trying for mild cases. Applying under occlusion or using a nail lacquer can help the medicine reach the nail better.
Injections: For more stubborn single‑nail problems, intralesional steroid injections (usually triamcinolone) into the nail matrix work well. They can be uncomfortable but often give clearer, faster improvement than topicals.
Systemic options: When many nails are affected or you have skin/joint disease, doctors may prescribe methotrexate, cyclosporine, acitretin, or biologic drugs (like TNF, IL‑17, or IL‑23 inhibitors). These treatments can significantly improve nails because they calm the immune system. Discuss risks and monitoring with your clinician.
Check for fungal infection: Onychomycosis can mimic or coexist with nail psoriasis. If your nails are very thick, crumbly, or discolored, your doctor may recommend a lab test (KOH or culture) before treatment.
Everyday nail care tips: Keep nails short and file rough edges. Avoid aggressive manicures, nail-biting, and acrylics. Moisturize cuticles and nail folds daily. Wear gloves for wet work and avoid trauma — even small knocks can flare psoriasis in nails. Use gentle nail tools and disinfect them regularly.
When to see a dermatologist: If nails hurt, interfere with daily tasks, or don’t improve after several months of home care, get a dermatologist consult. If you have joint pain or many nails involved, talk to your provider about systemic therapy options.
Managing expectations helps — improvements are gradual, but with the right mix of medical treatment and nail care, most people see noticeable progress and less damage over time.

 Apr, 27 2023
Apr, 27 2023